Tibial nerve pain is characterized by lesions of various etiology, which leads to dysfunction of the muscular apparatus of the lower leg, foot, and fingers. The main reason is traumatic, mechanical, or infectious damage to the nerves of the lower extremities. The pathological process leads to the development of pain syndrome, the formation of puffiness, increased sensitivity and spasm of the muscles of the leg and foot, as well as other neurotrophic disorders.
Some of their symptoms coincide, as well as individual methods of treatment. However, accurate diagnosis is essential to achieve the best results in nerve repair. To do this, you need to identify and eliminate the root cause of the problem.
Causes
The tibial nerve is an extension of the sciatic nerve. Its damage is possible in the following cases:
- Injuries of the lower extremities of various etiologies (fracture, dislocation or sprain of the ankle, rupture of tendons, sprain of the ligaments of the foot). Traumatic factors and edema caused by them lead to direct damage or compression of the tibial nerve pain, which leads to a violation of the transmission of nerve impulses.
- Deformation changes in the foot (flat feet, valgus).
- Squeezing the feet or their uncomfortable position for a long time, for example, when squeezing the lower limbs with a heavy object.
- Diseases of the knee joint and ankle (arthritis, arthrosis).
- Disorders in the functioning of the endocrine system, thyroid diseases, diabetes mellitus.
- Tumor lesions of the tibial nerve, benign and malignant.
- Violation of blood flow to the lower leg and feet of the lower extremities (vasculitis).
- Poisoning of the body with toxic and chemical compounds, including alcohol-containing products.
- Inflammatory pathologies of infectious etiology of various localization, including multiple lesions of nerve fibers.
- Long-term therapy with drugs, the action of which negatively affects the functioning of the central nervous system.
- Decrease in the protective properties of the body.
- Harmful working conditions.
- Malnutrition of the tissues of the lower leg and foot.
- Long-term exposure to low temperatures on the lower extremities.
- Improper nutrition, as a result of which the intake of B vitamins into the body is reduced.
- Pathological processes affect the spinal column.
The risk group includes people:
- professionally engaged in various sports;
- with working conditions that require constant standing, including walking;
- prone to overweight or obesity – a large load on the lower limbs increases the risk of dysfunction of the tibial nerve pain;
- choosing the wrong footwear: high heels, thin soles.
Symptoms of Tibial Nerve Pain
Neuropathy is accompanied by a clinical manifestation of severity, which depends on the degree of damage to the nerve fibers.
Dysfunction of the nerve can be recognized by impaired flexion of the foot, motor ability of the fingers. When walking, the foot is incorrectly positioned – the emphasis goes on the heel. The muscular apparatus of the lower leg and foot has signs of obvious atrophy and deformation.
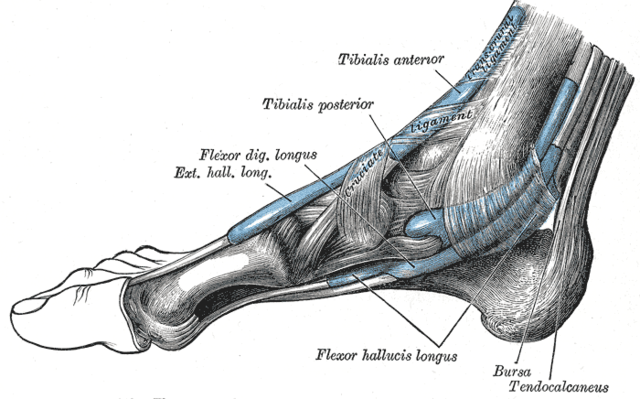
In the case of a traumatic origin of neuropathy, edema forms in the ankle area, blood flow is disturbed, tissue sensitivity increases, there is a pronounced pain syndrome, which increases when touching the damaged areas.
If the cause of the neuropathy of the nerve is endocrine disorders, infectious lesions, the patient loses sensitivity in the area of the lower leg and foot of the lower extremities. The pain syndrome persists and can have different natures and severity.
The pain increases with walking and physical exertion. The patient may experience involuntary contractions of individual muscles or a convulsive syndrome involving the lower extremities.
In addition, the patient is worried about neuro-trophic disorders, such as dryness of the epidermis in the lower leg and feet, keratinization of the upper layer of the dermis, brittle nails, pallor of the skin and a decrease in local temperature, increased sweating.
Diagnostics of the tibial Nerve
Tibial nerve belongs to the group of mononeuropathy of the extremities. The clinical picture of pathology is characteristic of dysfunctions of the musculoskeletal system and has a traumatic nature, and therefore, it is subject to joint observation and control by specialists in the field of neurology and traumatology.
The first step in making a diagnosis is to interview the patient about injuries to the lower extremities, working conditions, as well as the peculiarities of the clinical picture, and the presence of other diseases that can affect the normal performance of the nervous system.
After that, the patient is examined to identify atrophic and neurotrophic changes in the lower leg and foot.
Based on the data obtained, an initial diagnosis is made, which is confirmed by instrumental studies, using one of the following methods:
- ultrasound diagnostics of the lower extremities;
- electromyography is a research method that allows you to determine the performance of the muscular apparatus of the lower leg and foot;
- X-ray diagnostics if indicated, for example, with fractures;
- blockade of trigger points is a therapeutic and prophylactic method involving the introduction of a drug into the affected areas of the lower extremities, which allows you to determine the degree of nerve damage;
- CT and MRI are used as additional diagnostic methods when, when using other methods, there is not enough data to make a diagnosis.
Therapy
The initial stage in treatment is the therapy of pathology, the root cause of the dysfunction of nerve fibers. For example, for endocrine disorders of the system, hormones are prescribed, for diabetes mellitus, medications are prescribed to normalize blood sugar levels. With a lack of B vitamins, intravenous administration of drugs with vitamins B1, B6, and B12 is indicated, which will improve the nutritional capacity of the tissues of the nervous system.
To reduce the severity of the feeling of pain, to resume physical activity, the patient is prescribed special orthopedic shoes or insoles. The choice is made in accordance with the localization of the lesion of the nerve fibers.
With severe pain, pronounced edema as a result of pinched nerve endings, blockades are performed with the introduction of analgesics (Analgin, Novocain) and anti-inflammatory nonsteroidal drugs (Ibuprofen, Dikroberil). Less commonly, steroids (hydrocortisone) or antidepressants (amitriptyline) are used.
In case of trophic disorders of surface tissues, re-agents (Solcoseryl, Actovegin) are recommended, the action of which is aimed at renewing cellular structures.
To suppress nervous excitability, anticholinesterase drugs (Ipidacrine) are used.
To restore performance and strengthen the muscular apparatus of the ankle, normalize blood flow, physiotherapeutic methods of therapy (electrophoresis, magnetotherapy, shock wave therapy), exercise therapy and massage sessions are shown.
Surgical intervention is necessary in the absence of efficacy from conservative therapy, nerve damage, adhesion formation, impaired sensitivity of the lower extremities and severe pain syndrome. The operation is performed by a neurosurgeon.
Shockwave Therapy
One of the modern and effective methods of physiotherapy is the shock wave method. It is carried out using a special apparatus that directs targeted acoustic waves of various frequencies to the damaged areas. The penetration depth of such waves is up to 4 cm.
This method allows you to improve the flow of blood with nutrients to the lower leg and foot, normalize metabolic processes, loosen neoplasms and reduce the severity of pain.
Shock wave therapy is used as a prophylactic and therapeutic one, in a course of 5 to 10 procedures with a break of 3-7 days between them.
The advantages of this method are:
- non-invasiveness of the procedure;
- a short course of therapy;
- the duration of one session is from 10 to 20 minutes;
- the possibility of simultaneous exposure to several damaged areas;
- pain reduction occurs after 2-3 sessions;
- long lasting effect.
This method is not applicable to patients with bleeding disorders, oncology, acute infectious pathologies, hypertension. UHT is also contraindicated in children under 14 years of age and in patients with a pacemaker.
Tibial nerve pain is characterized by the impaired performance of the muscular apparatus of the foot and lower leg, which leads to gradual tissue atrophy. It is characterized by pain, impaired walking, and foot placement. For treatment, the therapy of pathology-root causes is carried out, as well as medications are prescribed to relieve pain syndrome and physiotherapy procedures. Surgical intervention is carried out according to indications.
Reference
| Name | Website URL |
| Wikipedia | CLICK HERE TO VISIT |






